Therapy vs. Medication for Prenatal Depression
-
1 in 5 pregnant individuals in the U.S. experience prenatal depression annually. Symptoms like sadness, anxiety, and fatigue can disrupt daily life and preparations for the baby.
-
Untreated prenatal depression can lead to serious risks, including preeclampsia, missed prenatal care, preterm birth, and low birth weight.
-
Treatment options include therapy (e.g., CBT or IPT) and medication (commonly SSRIs like sertraline). Both approaches are effective, and many benefit from combining the two.
Quick Overview: Therapy vs. Medication
-
Therapy: Non-medicated, focuses on thought patterns and relationships, with no fetal risks.
-
Medication: Balances brain chemicals, effective for severe cases, with minimal risks to the baby.
Key takeaway: Work with your healthcare provider to choose the right treatment based on your symptoms and personal needs. Untreated depression poses greater risks than most treatment options.
Treatment of Depression in Pregnancy (Treatment of Antenatal Depression)
How Therapy Works for Prenatal Depression
Therapy provides a non-medicated way to address prenatal depression by focusing on reshaping negative thought patterns and improving strained relationships. Two widely used methods are Cognitive Behavioral Therapy (CBT) and Interpersonal Psychotherapy (IPT).
Common Therapy Approaches
Cognitive Behavioral Therapy (CBT) zeroes in on the link between thoughts and emotions. It helps expectant mothers identify and replace harmful beliefs - like "I'll be a terrible mother" - with healthier, more balanced perspectives. As described by the National Institute of Mental Health:
"With CBT, people learn to challenge and change unhelpful thoughts and behaviors to improve their depressive and anxious feelings."
Meanwhile, Interpersonal Psychotherapy (IPT) takes a relationship-focused approach. Pregnancy often brings major life changes and role adjustments, which can strain relationships and contribute to depression. IPT works to strengthen communication skills and build supportive social connections during this transitional period.
Research backs the effectiveness of these methods. For instance, in a clinical trial of brief IPT (MOMCare), only 6.1% of pregnant women receiving therapy developed Major Depressive Disorder by the end of pregnancy, compared to 26.1% of those receiving standard care.
Both CBT and IPT not only ease symptoms but also help mothers develop coping skills that extend well beyond pregnancy.
Benefits of Therapy
One of therapy's key advantages is its safety - it poses no physical risks to the mother or baby, unlike certain antidepressant medications that have been linked to neonatal respiratory problems. Many pregnant women lean toward therapy over medication due to concerns about potential impacts on their unborn child.
Therapeutic interventions have been shown to lower the risk of prenatal depression by up to 39% (absolute risk reduction: 1.3%–31.8%). A meta-analysis of CBT-based approaches revealed a medium effect size of -0.53 in reducing symptoms of depression. Beyond improving mental health, therapy has been associated with better pregnancy outcomes, such as higher birth weights and reduced rates of preterm delivery.
Both CBT and IPT can be offered one-on-one or in group settings. Group sessions, in particular, provide an opportunity for expectant mothers to connect with others going through similar struggles, fostering a sense of community and shared understanding.
|
Therapy Type |
Primary Focus |
Key Benefits |
|---|---|---|
|
Cognitive Behavioral Therapy (CBT) |
Identifying negative thoughts and managing stress responses |
Medium effect size (-0.53) in reducing symptoms |
|
Interpersonal Psychotherapy (IPT) |
Strengthening communication and social support |
Decreased depression rates from 26.1% to 6.1% in clinical trials |
How Medication Works for Prenatal Depression
Antidepressants play a key role in managing prenatal depression by balancing brain chemicals linked to mood regulation. While it can take 4–8 weeks for these medications to reach their full effect, some early signs of improvement - like better sleep, appetite, or focus - may appear sooner. Below, we’ll explore common medications used during pregnancy, along with their benefits and risks.
Common Antidepressant Medications
Selective Serotonin Reuptake Inhibitors (SSRIs), especially sertraline, are among the most commonly prescribed antidepressants for pregnant individuals due to their well-documented safety profile. Research shows that sertraline can boost response rates by 2.24 times and remission rates by 2.51 times compared to a placebo. The Society for Maternal-Fetal Medicine highlights:
"The available data consistently show that SSRI use during pregnancy is not associated with congenital anomalies, fetal growth problems, or long-term developmental problems."
For those managing bipolar disorder, decisions around mood stabilizers can be more complicated. Discontinuing these medications during pregnancy significantly increases the risk of relapse, shortening the time to recurrence from 28 weeks to just 2 weeks. However, some stabilizers, like lithium, carry higher risks. For example, lithium exposure during the first trimester has been linked to an adjusted relative risk of 2.25 for cardiac anomalies compared to lamotrigine.
Risks of Antidepressants During Pregnancy
All pregnancies carry a baseline 3% to 5% risk of birth defects, regardless of medication use. According to the National Institute of Mental Health, "the risk of birth defects and other problems for babies of mothers who take antidepressants during pregnancy is very low".
In some cases, newborns may experience neonatal adaptation syndrome, which can cause temporary symptoms like irritability, jitteriness, or respiratory issues. Observational studies have also linked antidepressant use to potential risks like preterm delivery and persistent pulmonary hypertension of the newborn (PPHN). However, these studies don’t establish a direct cause-and-effect relationship, as the severity of the untreated depression itself might influence these outcomes.
The risks of untreated depression during pregnancy often outweigh those of taking medication. Pregnant individuals who halt antidepressants face a 5 times higher risk of relapse compared to those who continue treatment. Abruptly stopping these medications is strongly discouraged, as it can lead to withdrawal symptoms and a heightened chance of relapse.
Therapy vs. Medication: Side-by-Side Comparison
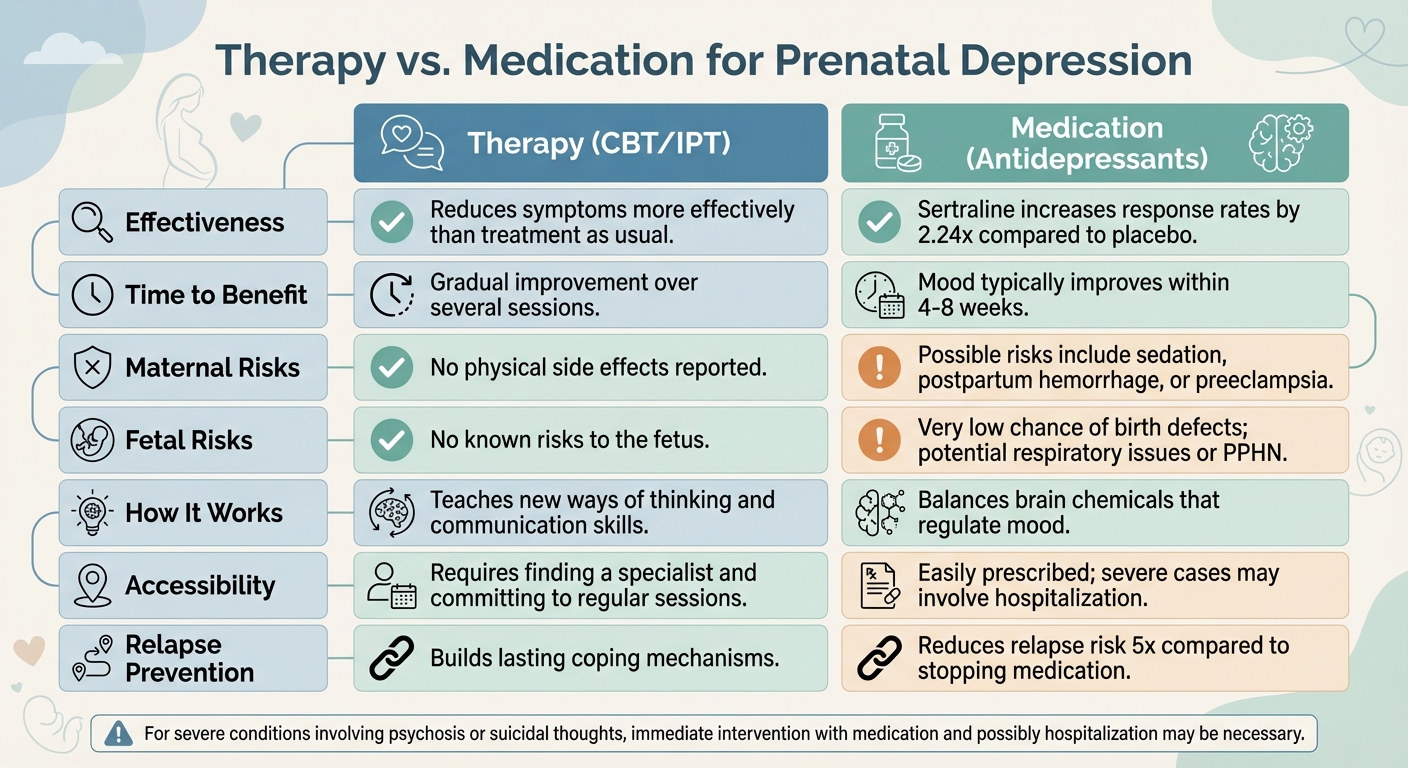
Therapy vs Medication for Prenatal Depression: Side-by-Side Comparison
Let's take a closer look at how therapy and medication stack up against each other. Neither approach can be labeled as universally better because the available evidence doesn't clearly favor one over the other. The best choice often depends on the individual's symptoms and personal circumstances. In fact, many treatment plans combine both therapy and medication for a more comprehensive approach.
Here's a breakdown of the key differences:
Comparison Table
|
Factor |
Therapy (CBT/IPT) |
Medication (Antidepressants) |
|---|---|---|
|
Effectiveness |
Reduces symptoms more effectively than treatment as usual |
Sertraline increases response rates by 2.24 times compared to placebo |
|
Time to Benefit |
Gradual improvement over several sessions |
Mood typically improves within 4–8 weeks |
|
Maternal Risks |
No physical side effects reported |
Possible risks include sedation, postpartum hemorrhage, or preeclampsia |
|
Fetal Risks |
No known risks to the fetus |
Very low chance of birth defects; potential respiratory issues or PPHN |
|
How It Works |
Focuses on teaching new ways of thinking and communication skills |
Helps balance brain chemicals that regulate mood |
|
Accessibility |
Requires finding a specialist and committing to regular sessions |
Easily prescribed; severe cases may involve hospitalization |
|
Relapse Prevention |
Builds lasting coping mechanisms |
Reduces relapse risk fivefold compared to stopping medication |
For severe conditions involving psychosis or suicidal thoughts, immediate intervention with medication and possibly hospitalization may be necessary.
Choosing the Right Treatment for You
Selecting the right treatment for prenatal depression involves considering factors like symptom severity, your mental health history, and how the condition affects your daily life. It's essential to work closely with your healthcare provider to weigh the risks of untreated depression against any concerns about medication. As Dr. Meir Steiner from McMaster University puts it:
"The decision to use antidepressants in pregnancy... should also take into account the stress and burden of illness that the pregnant woman is under."
Your provider may also check for underlying issues, such as thyroid disease or anemia, which can mimic depression symptoms. Additionally, reviewing any previous treatments can help guide your approach.
When Therapy Is the Best Option
For mild to moderate prenatal depression, therapy is often the first recommendation. If you’re feeling persistently sad or anxious but can still manage most of your daily responsibilities, approaches like Cognitive Behavioral Therapy (CBT) or Interpersonal Therapy (IPT) can be effective. These therapies focus on building coping skills and addressing unhelpful thought patterns or relationship challenges - all without involving medications. Therapy is especially beneficial if you have a strong support system and want to focus on behavioral and emotional strategies.
When Medication May Be Needed
In cases of moderate to severe depression, medication may become necessary, particularly if therapy alone isn’t enough. If you’re struggling to care for yourself, experiencing thoughts of self-harm, or facing psychosis, immediate medical attention - and possibly hospitalization - is crucial. Antidepressants generally take 4 to 8 weeks to reach full effectiveness, though some improvements, like better sleep or appetite, may appear sooner. Many women find that combining medication with therapy helps address both the biological and behavioral aspects of depression.
Adding Self-Care to Your Treatment Plan
Self-care can play a powerful role in enhancing any treatment plan. Activities like regular exercise can help boost your mood during pregnancy. Bright light therapy and omega-3 fatty acid supplements have also shown promise as safe, complementary options. Building a support network and engaging in activities that bring you joy can further help manage prenatal depression.
For added support, Rumbly offers pregnancy wellness boxes tailored to each trimester. Starting at $29.00, these curated boxes include self-care items and practical essentials. For a more comprehensive option, the Modern Mom-to-Be Box, priced at $78.00, provides a thoughtful blend of wellness and everyday necessities. Whether you choose therapy, medication, or a combination of both, prioritizing your self-care can make a meaningful difference during your pregnancy journey.
Conclusion
Managing prenatal depression involves understanding your symptoms, considering your personal history, and working closely with your healthcare provider to make informed choices. Whether you lean toward therapy or medication, the goal is to find the safest and most effective treatment for your situation.
For mild to moderate symptoms, therapies like CBT and IPT can be highly effective. However, severe cases may require antidepressants to address the condition adequately. Leaving depression untreated poses risks to both you and your baby, highlighting the importance of professional care. Alongside medical treatment, incorporating self-care practices can further support recovery.
Self-care plays a vital role in improving mental health. Activities like regular exercise, building a strong support system, and accessing immediate resources - such as the National Maternal Mental Health Hotline (1-833-852-6262)- can help alleviate symptoms. This holistic approach aligns with the balanced strategies discussed earlier.
It's crucial to remember that perinatal depression is a medical condition, not a personal shortcoming. Seeking help is a powerful step toward safeguarding your well-being and your baby’s health.
If you’re looking for ways to nurture yourself during this time, check out Rumbly's curated pregnancy boxes. They’re designed to support the self-care and wellness of expectant mothers.
Sending hugs,
rumbly 💜
FAQs
How do CBT and IPT differ in treating prenatal depression?
When it comes to managing prenatal depression, Cognitive Behavioral Therapy (CBT) and Interpersonal Therapy (IPT) offer two distinct paths to relief, each with its own focus and benefits.
CBT works by targeting negative thought patterns and behaviors. Through this approach, individuals learn to identify these thoughts and replace them with healthier, more constructive ones. The results? A moderate improvement in symptoms that can often last up to six months after completing treatment.
IPT, however, takes a different approach. It emphasizes strengthening interpersonal relationships and building social support networks. This method tends to provide a quicker reduction in symptoms, making it appealing for those seeking more immediate relief. That said, the evidence backing IPT's effectiveness isn't as strong as it is for CBT.
Choosing between these therapies often comes down to what you need most - longer-term benefits or faster relief. A healthcare provider can guide you in deciding which option aligns better with your situation and preferences. Both approaches have their strengths, and the right choice depends on your unique circumstances.
Are SSRIs safe to use during pregnancy?
SSRIs are widely regarded as safe for use during pregnancy. Studies indicate that these medications generally do not raise the risk of birth defects. On the other hand, leaving depression untreated during pregnancy can lead to serious issues like preterm birth or low birth weight, which may pose greater risks to both the mother and the baby.
That said, there are rare instances where SSRIs have been associated with conditions in newborns, such as heart or lung complications. Choosing whether to continue SSRIs during pregnancy is a decision that should be made carefully with your healthcare provider. Together, you can weigh the potential benefits and risks to find the best path forward for both you and your baby.
When is medication recommended instead of therapy for prenatal depression?
When prenatal depression becomes severe or starts to interfere with daily life, medication might be considered - especially if therapy alone isn’t offering enough relief. This decision is usually made after careful discussion with a healthcare provider, who will assess both the potential benefits and risks for the mother and baby.
Sometimes, a combination of therapy and medication can provide better outcomes. It’s important to talk openly with your doctor to find the safest and most effective way to manage prenatal depression.






